Mental health advocates are fighting Gov. Chris Sununu’s two-part proposal to force hospitals to give the state more emergency psychiatric hospital beds and extend the time the state can hold someone in an emergency room for involuntary admission.
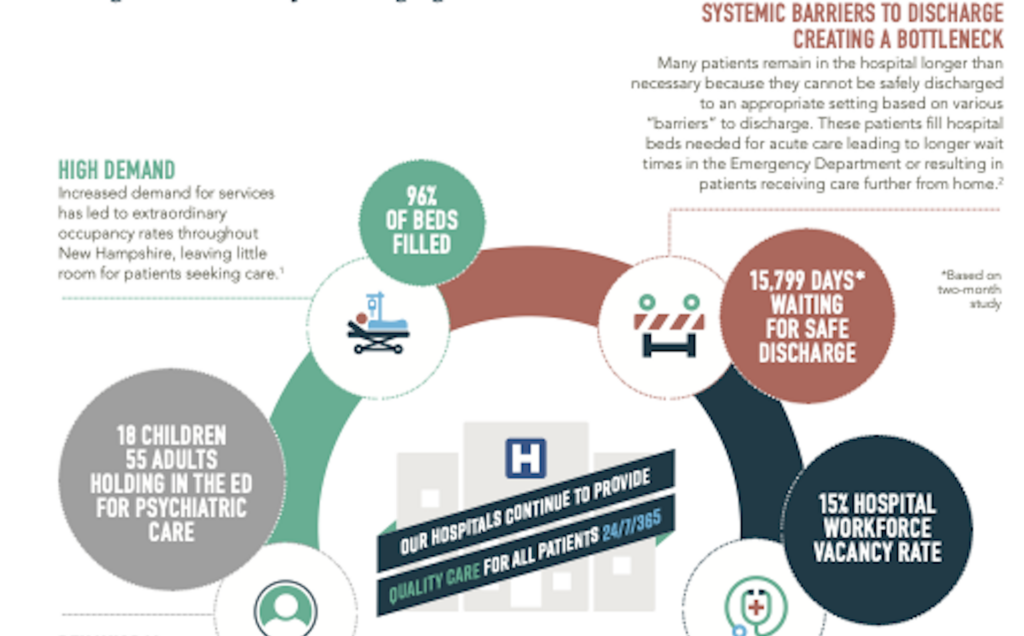
Among those pushing back is the New Hampshire Hospital Association, which says hospitals are already short beds because of workforce challenges and the inability to discharge patients to long-term care because those facilities are also full. In a recent media briefing, the association listed high numbers of adults and children waiting in hospital emergency rooms for days or weeks for admission for psychiatric care.
Steve Ahnen, president and chief executive officer of the New Hampshire Hospital Association, said Sununu’s proposal “is not the answer and it will only enshrine a broken system” of using emergency departments to detain patients because the state has too few mental health beds.
“We’ve had a behavioral health crisis and ED boarding wait list for the last decade,” Ahnen said. “That needs to end. We’ve been willing to sit down to resolve this matter, but the state has never put forth a proposal that would end the ED boarding crisis. That needs to happen now.”
Sununu’s request in House Bill 2 was a surprise to the hospital association and other mental health advocates.
If the measure is adopted by the Legislature, the hospitals would have to provide the state two to nine of its beds, depending on their size, for patients the state is involuntarily holding in emergency rooms until a bed opens. And, the Department of Health and Human Services would no longer have to “immediately” transfer a patient from an emergency room to a hospital, as the law requires now. The department would be able to hold someone until a hospital bed in the patient’s community became available.
The ACLU of New Hampshire is concerned about that timing request.
“We have initial concerns that this language might be interpreted to permit indefinite emergency room boarding in New Hampshire where individuals are not promptly getting the treatment they need,” said legal director Gilles Bissonnette. “We hope the commissioner (of Health and Human Services) and the hospitals will engage with us and other stakeholders to address these concerns.”
The Disability Rights Center-NH is criticizing what it calls Sununu’s “fixation on expanding inpatient psychiatric beds.” It noted too that there are often dozens of patients at New Hampshire Hospital who are ready for discharge but remain at the hospital because there is insufficient supports and housing in the community to help them transition to independent living.
As of last week, New Hampshire Hospital had closed 31 of its 184 beds due to staffing challenges, renovations, or both, Department of Health and Human Services spokesperson Jake Leon said in an email.
Monday there were 28 adults being held in emergency rooms and seven in correctional facilities, according to the state’s tracker.
“Rather than continue to inappropriately warehouse people in facilities, (New Hampshire) needs to make long-term investments in community-based supports and services that enable people to receive care when they need it, where they need it, while maintaining their homes, jobs, and other family and community connections,” said Karen Rosenberg, policy director for DRC-NH, in an email.
Hospitals didn’t bite in 2021 when the state offered them $200,000 for every bed they made available for the 20 to 35 adult psychiatric patients languishing in emergency rooms on any given day. With HB 2, Sununu wants to make that request a requirement.
He blasted hospitals when asked about his request, which he did not highlight in his budget address to lawmakers. In his response to media questions, Sununu referenced a federal lawsuit over the state’s emergency room boarding practice brought by ACLU-NH in 2018 and joined a year later by several hospitals.
“The hospitals have been extremely clear that they don’t want to be part of the mental health solution,” Sununu said. “They should be ashamed. This latest lawsuit by the hospitals is a horrible example of one of our most important community institutions, such as a hospital, essentially saying that mental health is not a health issue. And that’s wrong. They’re absolutely wrong.”
The Department of Health and Human Services did not request funding for more beds but is backing Sununu’s proposal, Leon said.
“The Department supports any proposal that will allow the State to partner with private entities to increase capacity to serve this vulnerable population,” Leon said in an email. “The request aligns with the state’s focus on deinstitutionalization of mental health services and ensuring patients receive care in community-based settings.”
Neither the department nor Sununu have said how the state will compensate hospitals for the new beds, which the hospital association has put at about 100 and Leon said would be closer to 130. The state currently has 62 beds in the community, outside those at New Hampshire Hospital, available for patients involuntarily admitted because they are deemed a danger to themselves or others. That’s too few for everyone being held in an emergency room or correctional facility.
Under Sununu’s request, hospitals with 25 or fewer licensed patient beds would have to provide the state two beds for involuntary admissions as a condition of their state license to operate. That number would increase to four beds for hospitals with between 25 and 100 beds and to six beds for those with 100 to 200 beds. Hospitals with more than 400 beds would be required to make nine available to the state.
According to a list of hospitals and their bed count provided by Leon, Upper Connecticut Valley Hospital in Colebrook is the smallest with 16 beds and Dartmouth-Hitchcock Medical Center in Lebanon is the largest with just under 400 beds.
Ahnen warned a House legislative committee last week that forcing hospitals to expand their involuntary admission beds could exacerbate the state’s hospital staffing shortages because hospitals pay those workers more than the state.
Susan Stearns, executive director of NAMI NH, didn’t dispute the need for more emergency hospitalization beds, but said an increase in other beds is critical, including those in affordable housing, transitional beds for those leaving the hospital, and crisis stabilization beds for people who need a safe setting and treatment but not a hospitalization.
“There are a lot of things wrong with emergency department boarding,” she said. “One of them is waiting for treatment. What other illness would you present with that you would wait for treatment for days in a medical facility? And we know that that delay can be harmful for some folks.”
In a statement, the Community Behavioral Health Association, which includes the state’s 10 community mental health centers, echoed that. The association asked the governor to increase their funding for the next two years by $30 million through a 21.5 to 23 percent increase in their Medicaid rate, primarily to pay competitive wages. Sununu has proposed a 3.1 percent increase.
“The 10 nonprofit mental health centers are partners with the state and the hospitals in managing the mental health system of care – and it is a system,” the statement read. “In fact, over the last several months, the (community mental health centers) have collectively opened nearly 50 new residential mental health beds that allow for the proper transition of patients from acute settings back into the community.”
The association reiterated its argument that a solution to a shortage of mental health services must include a strategy for expanding the workforce.
This story is courtesy of NH Bulletin under creative commons license. No changes have been made to the article.