
The warning drums have been beating for years about workforce shortages in health care and, while shortages persist, experts project some segments of health care could actually see a surplus of employees in the next decade. Yet that feast is expected to be accompanied by other health-care segments continuing to experience famine.
Health care is a major economic driver in NH, fueled by the state’s older population. When asked which sectors of health care are most affected by workforce shortages in the state, the most common refrain from those in the trenches is, “where aren’t we seeing shortages?”
Not enough nurses, not enough doctors and few techs and assistants are common challenges. Some hospitals even struggle to attract maintenance workers to fill the needs of their 24/7 operations.
“We are seeing shortages across the board,” says Sarah Currier, Dartmouth Hitchcock Health System’s vice president of workforce strategy. “Ten years ago we would post a job and there would be a hundred applicants and today we post a job and for a very similar position, we’ll see something along the lines of 11.”
Yet NH’s health-care industry may end up in better shape than other states in the coming years. RegisteredNurses.org analyzed future registered nursing employment estimates by the National Center for Health Workforce Analysis and found several states will face significant shortages of registered nurses by 2030 but not NH.
California is expected to be short the most registered nurses (45,500), while Alaska is projected to have the most job vacancies (22.7%). Texas, New Jersey, South Carolina, Georgia and South Dakota are expected to experience shortages as well, according to the site’s analysis. While NH cracked the top 10 for having the greatest difference between supply and demand for registered nurses, it is actually expected to have a slight surplus of 1,100 by 2030.
The Nursing Shortage
The promise of greener pastures is still a decade away. The current state of health-care employment is far bleaker. As of April, the number of full-time-equivalent employees budgeted in NH for nursing, behavioral health, rehabilitation, technical and senior leadership positions at 20 hospitals across the state was 21,427, according to a survey conducted by the NH Hospital Association. However, only 19,392 positions were staffed, leaving 2,035 vacancies or a total vacancy rate of 9.5%.
The need for nurses is highest nationwide and in NH, according to the survey. Vacancies for nurses in intensive care, operating rooms and anesthesia hover at around 15%.
 “Nursing would be our biggest [challenge] because it’s our biggest group of employees,” says Merryll Rosenfeld, vice president of human resources for Catholic Medical Center (CMC) in Manchester. And it’s not a pipeline issue.
“Nursing would be our biggest [challenge] because it’s our biggest group of employees,” says Merryll Rosenfeld, vice president of human resources for Catholic Medical Center (CMC) in Manchester. And it’s not a pipeline issue.
Jennifer Cassin, vice president of nursing for CMC, says there’s no shortage of new nursing graduates or students. CMC saw 600 students come through the hospital last year, as part of their training and hired 47. The challenge lies in the number of retirees leaving and a high turnover rate, particularly among new nurses.
“You tend to lose more in that first year or within the first couple of years following,” Cassin says, a trend that is particularly pronounced among millennials. “Once they get their experience, or their orientation as we call it, they’re looking to do relocation. They like to be travelers. They’re not afraid to move on in their careers and career advancement.”
Cassin says the shortages create scheduling challenges, exacerbating the long and non-traditional hours nurses work. And with higher pay available in nearby Boston, retention becomes an issue.
“A lot of them are going down to Boston because they could work three days a week and make oodles of money and then they come back home to New Hampshire,” Rosenfeld says. (See sidebar below.)
While Boston offers higher pay in general, “New Hampshire actually pays a little more,” than other Northern New England states, says Jason Hooper, nursing manager for MAS Medical Staffing, which specializes in traveling nurse programs and staffing health-care facilities.
More employers also are offering signing bonuses in certain nursing specialties, and, Hooper says, taking advantage of available federal stipends that can offset living costs for traveling nurses.
Mental Health Sector Challenges
Another health-care sector experiencing gaps is behavioral health. According to a NH Hospital Association survey, there is a 13.3% vacancy rate among behavioral health nurses and a 13.5% vacancy rate for behavioral health clinicians.
While the survey didn’t specify this, the state has a shortage of practicing psychiatrists. While the number of active licenses for psychologists in the state increased from 559 in FY 2017 to 639 in FY 2018, according to NH Employment Security, there were only 60 psychiatrists in NH in 2017. (Psychiatrists are medical doctors who can prescribe medication.) By comparison, there were 910 family and general practitioners employed in NH.
“There’s a national shortage of psychiatrists,” says William Torrey, professor and vice chair for clinical services for the department of psychiatry at Dartmouth’s Geisel School of Medicine and Dartmouth-Hitchcock. “Studies show that most counties in the country don’t have enough psychiatrists.”
There are many reasons, Torrey says. First, more than 60% of psychiatrists are 60 or older. This means many of them are retiring or cutting back hours, reducing overall capacity in the mental health system. Further, he says, there’s a growing recognition of the need for psychiatrists in nursing homes, jails and other non-traditional settings.
Adding to the demand for services are such advancements as telemedicine that provide patients in rural areas with greater access to services. “I’ve taken care of people in a nursing home in Rutland from my office here at DHMC,” Torrey says, explaining that while it makes it easier for patients to access his services, it also creates more competition for his time. “There’s just a lot more demand for the service,” he notes.
Psychiatrists historically have been underpaid by insurance, adding to the shortage woes. “Right now, if we hire a psychiatrist here and keep them really busy doing outpatient work, they cost almost twice as much as they bring in,” Torrey says. “That means that a substantial percentage of the psychiatrists—I think about 40 percent of psychiatrists—do not take insurance because insurance companies make it really difficult to get paid and they’re not paying enough.” That, in turn, cuts down on how many psychiatrists are available to work at community mental health centers, hospitals and other facilities that have to take insurance, he says.
Even putting reimbursement rates aside, psychiatrists, nationally and in NH, simply get paid less than other practitioners, making it hard to recruit new students into the field. According to NH Employment Security, psychiatrists make an average of $108 per hour. Experience raises that figure to $128 per hour, while entry level psychiatrists make roughly $71 per hour.
By comparison, general practitioners make an average of $127 per hour, internists, $133 and surgeons, $148.
That is starting to change and psychiatrists are starting to command better salaries, Torrey says, which should help attract more medical students into psychiatry. Also helping to attract students is increased research in brain science as well as a diminishing stigma around mental health.
But sometimes that’s not enough. “The state has lost a lot of inpatient hospital capacity over the years with hospitals closing down inpatient units,” Torrey says. “You need to have jobs for people to stay in state.”
Technician Shortages Soar
Another area experiencing shortages is pharmacy technicians with vacancy rates at 16.6%—the most vacancies of all the positions surveyed by the NH Hospital Administration.
Nurses and medical techs need to be licensed or credentialed and the cost of their education can be out of reach for some who may decide to pursue other career paths, Dartmouth-Hitchcock’s Currier says.
For example, someone looking to be a licensed nursing assistant has to pay for classes that cost at least $1,300 to $1,500.
Then he or she has to take and pay for an exam and wait for the results. Then they have to pay for the licensing itself and wait through that process to find out if they will be licensed. Then after that, they wait through a background check, they are hired and can get to work—for roughly $15 per hour.
“I can go into Kohl’s [department store] and there’s a little sign that says ‘text this number if you’re interested in an interview’ and I can text that number in this dressing room and they will offer me an interview and a job before I leave the store,” Currier says. “In short, for all the time, effort and expense of getting one of these lower-skilled tech jobs the person thinks, ‘I could’ve taken a job elsewhere for $15.’”
What’s Behind the Current Shortages
Currier and others point to a number of factors leading to the shortages facing NH’s health-care industry: aging population, growing competition for a dwindling number of available qualified workers, and ease of mobility that allows new graduates to get out of Dodge and take a job elsewhere.
And there are systemic factors at play here too, says Currier, including low Medicaid reimbursement rates that result in lower pay for behavioral and mental health practitioners as compared to other providers; strict regulations; and not enough affordable housing, public transportation and high-speed internet to attract and retain young professionals lured by the bright lights, bigger paychecks and better amenities in Boston and other cities. “It’s kind of a perfect storm,” says Currier.
Gains and Surpluses Ahead
Demand for health-care workers will continue. By 2026, the health-care and social assistance sectors are expected to see the highest job gains, with an increase of 14,189 jobs, and contribute roughly one-third of new jobs in the state, according to the most recent NH Employment Projections by Industry and Occupation report, conducted by NH Employment Security.
This is an expected 15.7% growth. The next fastest-growing sector—professional, scientific and technical services—will see an employment gain of 13.7%.
And while workforce shortages will persist in some areas of health care, others are expected to see a surplus. By 2030, it’s projected there will be a 5.4% surplus of registered nurses but a 37% shortfall of LPNs in NH, according to a 2017 report issued by the U.S. Department of Health and Human Services, Health Resources and Services Administration conducted by the National Center for Health Workforce Analysis.
There also will be a projected surplus of primary care practitioners across the board by 2025, according to another DHHS report analyzing projections for that sector. The report projects NH will have a 4.5% surplus of primary care physicians; a 62.5% surplus of primary care physicians assistants; and a 160.7% surplus of primary care nurse practitioners.
While a potential surplus of nurses and doctors will likely carry its own challenges; for the time being, the health-care industry must contend with current shortages. Providers across the state aren’t throwing up their hands in surrender, though. Officials in the state are developing ways to combat the trend and collaborating to meet community needs.
The Pipeline
Colleges specializing in health-care programming are encouraging students and potential students to look to nursing and other high-demand fields in health care. Alfred Williams, president of River Valley Community College, says one in 10 graduates from the community college system is in a nursing field.
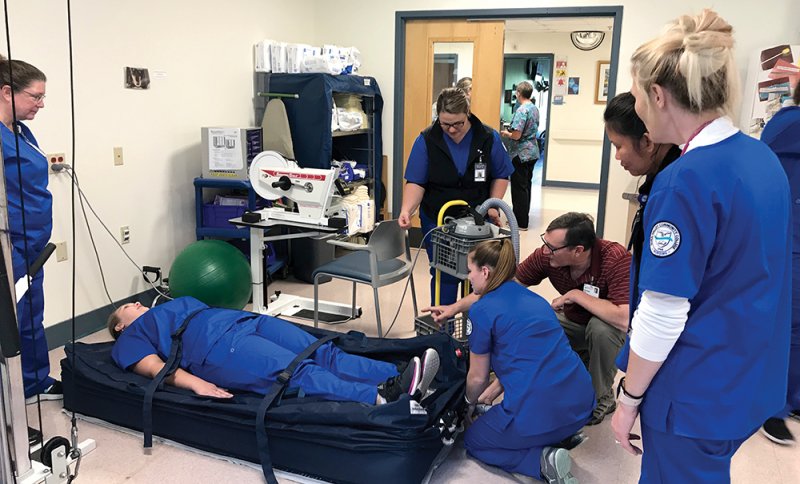
Nursing students at River Valley Community College. Courtesy photo.
“The demand is so high,” he notes, adding that some are shocked to find out that 10% of graduates of the community college system are going into nursing careers. “There’s no other major that even comes close to that.”
Furthermore, 97% of the community college nursing grads end up with a job in NH, he says. “It’s a great program for students because in two years, they end up getting jobs as RNs and then a lot of them complete their bachelor’s degrees while they’re working.”
Competition to get into these nursing programs is high as spaces are limited. “The programs are highly selective and in high demand and it’s hard to grow,” Williams says. “You can’t really grow the programs. We could double the amount of students in our nursing program; the problem is that you need clinical sites. There’s only so many clinical sites in the state. And also you need the faculty, because we’re training people to deal with people’s lives and so there’s criteria that needs to be met.”
A simple Google search for nursing faculty jobs in NH produced a list of more 70 open positions, many of which require a master’s or bachelor’s in addition to experience and licensure.
Finding LNA faculty is equally tough, but Currier of Dartmouth says some regulatory tweaks could make a difference. “We can’t get out of our own way. The current law around who can teach a licensed nursing-assistant-training program requires that the instructor have long-term care in their background,” she says, explaining even if she had a nurse with 25 years of experience working in an acute care hospital and with an aging patient population, he or she wouldn’t be eligible to teach.
“It’s almost impossible to get that person approved as an instructor” because he or she had never worked in a long-term care facility. “Finding ways to solve some of that would be great.”
Samantha O’Neill, vice chair of the NH Board of Nursing, responsible for approving nursing program educators, says this is an issue with which its board regularly grapples.
“We want to make sure there’s a balance of meeting the needs and having safe patient care,” says O’Neill, who also serves as vice president of human resources for Portsmouth Regional Hospital. “We want to make sure that professors teaching either LNA courses or nursing courses have the appropriate experience.”
With limited slots for nursing courses and a perennial need for more faculty, Williams says River Valley offers students an alternative route into health care. “Our bread and butter is the allied health fields,” he says. “Because the nursing class fills up and has limited spots, we try to find other interests and other pathways,” for students.
One of those pathways involves starting as an LNA and then continuing to take classes and training to become an LPN and then a registered nurse. The college also offers certificate programs to become medical administrative assistants or medical assistants. It also offers an associate degree for medical laboratory technicians, a program expanding by one new faculty member this year. “We’ve been running a class of 12 students every year but the demand is for 18 to 22 students because the jobs are there,” Williams says.
Other programs growing in popularity include occupational, physical and respiratory therapy. “Students who graduate in respiratory therapy are making over $50,000 coming out of the program,” Williams says. “It’s not just nursing that can lead to these really high salaries.”
Colleges are offering more career pathways by partnering with local hospitals on creating apprenticeship programs. White Mountain Community College recently developed a medical assistant apprenticeship program with several area hospitals.
The idea is to quickly produce an initial cohort of medical assistants to meet hiring needs. In some cases, hospitals had positions that went unfilled for 18 months, according to White Mountain Community College officials. Based on an “earn-while-you-learn” model, students get paid to go to school and instead of going through a two-year certificate program, they earn their certificates within 12 to 15 weeks.
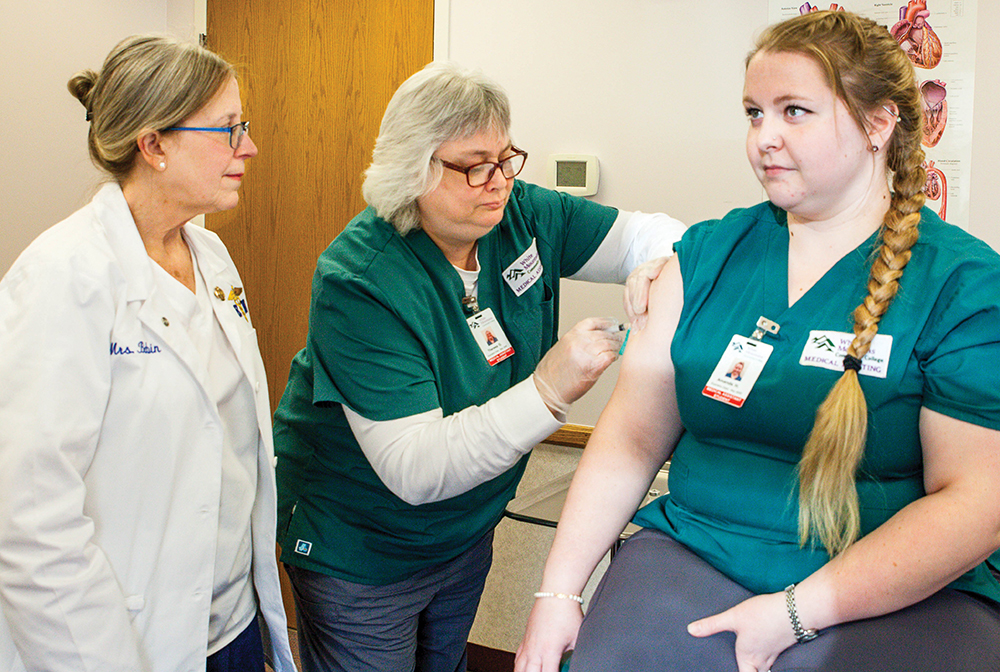
Students gain hands-on experience at White Mountain Community College’s certified clinical medical assistant apprenticeship program. Courtesy photo.
“Yes, it’s intense,” says Chuck Lloyd, president of White Mountain Community College, “but it’s done after that period. You’ve got your hours in and you’re back on the job. So shifting careers for some of these folks happens a lot quicker.”
Tamara Ann Roberge, coordinator for workforce development at White Mountain Community College, says the apprenticeship program plays a key role in attracting people who might otherwise be shut out by the expense or time needed to get licensed.
“For a lot of people in North Country, college is not in their horizon,” Roberge says. The apprenticeship program “has helped open up some avenues for people who might not have considered college. … Finding different ways of educating people while attaining those skills needed by the employers is a big deal.”
Roberge says the college is developing training programs specific to individual hospitals so that new recruits and current employees can upgrade their skills and earn while they learn.
Dartmouth Hitchcock is building partnerships with local colleges, including Colby Sawyer and River Valley to enhance their apprenticeship program. “We’re trying to build a combination, work and education super highway with lots of exit and on ramps that allow people to come in, dial up and dial back their career in a way that fits them and keeps them working,” Currier says.
Roberge says more grants to help offset the cost of training would allow the apprenticeship model to thrive.
It is also essential to engage students at a younger age and make them aware of careers in health care, says Lloyd. White Mountain Community College is using funds from the GEAR UP grant to educate middle school students about health-care careers. (GEAR UP is a federal grant program designed to increase the number of low-income students prepared to enter and succeed in post-secondary education.)
“By the time you get to high school, you’re starting to work with your school counselors to really choose a path and take the correct courses that are going to align with the prerequisites for those programs,” Lloyd says, adding that students really begin to think about what they want to be, when they are in the sixth or seventh grade. “It’s important to get on a pathway at that point.”
Legislative Fixes
The challenges of recruiting health-care professionals in NH go well beyond paycheck and education. Lack of affordable housing, little or no available public transportation and limited broadband are all barriers to recruiting and retaining workers. “This is really a multisystem failure in some ways,” Currier says, explaining she can present a compelling case for taking a job in NH until people look at housing prices.
According to the most recent NH Housing Finance Authority survey, the average monthly rent for a two-bedroom unit with utilities is $1,296. This has increased 19% in the last five years and it is the fifth consecutive year that rents have increased statewide.
The survey found that NH’s vacancy rate for two-bedroom units stands at 1.96%. In comparison, the U.S. vacancy rate is 7% and 5.1% in the Northeast. Further, a vacancy rate of 4% to 5% is considered a balanced market for supply and demand. Vacancies are particularly low in the southern counties of Hillsborough, Merrimack, Rockingham and Strafford, as well as in the communities of Hanover and Lebanon in the Upper Valley. The majority of large hospitals in the state are located near these areas.
Currier says while there are individuals, organizations, agencies and businesses working on the housing issue, they are doing so in silos. “We are a small state that feels like we have to solve everything locally. A lot of organizations out there are working on pieces of this problem, but … less gets done because we’re all trying to farm it individually with small dollars. I would love to see us find a way to come together with a solution around some housing.”
Meanwhile, hospitals are looking at ways to retain the existing workforce. Rosenfeld and Cassin at CMC are examining ways to promote employees, and also stave off compassion fatigue and burnout, which can lead to higher turnover.
To that end, CMC offers pastoral care to staff and allows nurses some level of self-scheduling to mitigate stress. “It’s finding that level of what is work-life balance,” Cassin says. CMC also helps staff debrief after a stressful day by speaking with a group about difficult, complex patient situations and getting feedback and support.
Further, hospitals are looking for ways for these initial incentives to turn into long-term benefits for both the employee and the organization. For example, several hospitals now offer tuition assistance to earn advanced certificates and degrees as well as creating pathways for advancement within the organization.
Portsmouth Regional Hospital offers tuition reimbursement and loan assistance programs to LNAs and promotes form within when possible, O’Neill says. “We’re trying to keep nurses challenged and advance their career if they so desire,” she notes.
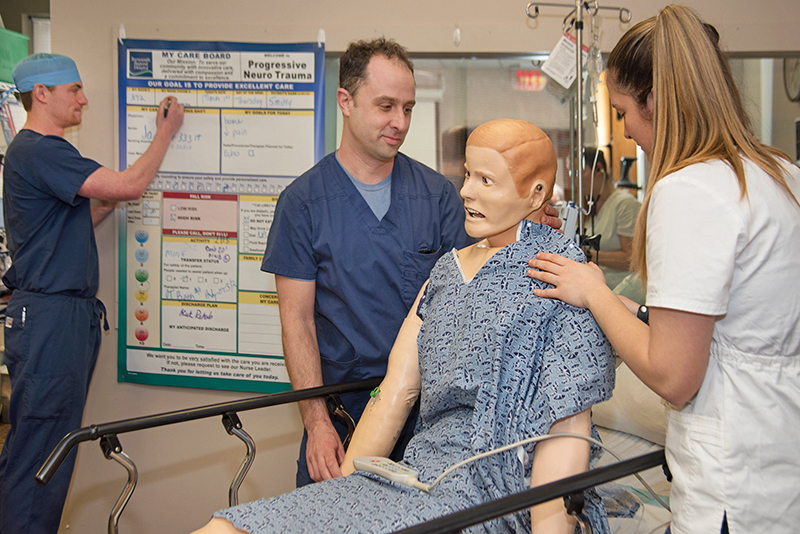
Nurses participate in the StaRN program, a nurse residency program specifically designed for new graduate nurses. The program is offered through Portsmouth Regional Hospital. Courtesy photo.
Looking to the Future
Increasingly, health-care centers are building partnerships to address workforce issues. Earlier this year, hospitals and clinics across the state formed a behavioral health collaborative to discuss the challenges they are facing and to develop a set of best practices.
Also this year, the University of NH became a Project ECHO hub and launched Partnership for Academic Clinical Telepractice (PACT).
Marcy Doyle, clinical and quality improvement director for the Institute for Health Policy and Practice NH Citizens Health Initiative, and an adjunct professor of nursing at UNH, says the goal is to bring together interdisciplinary specialists and community-based practitioners using web conferencing technology along with UNH’s nurse practitioner students. Doyle explains that during these sessions, a de-identified patient case in NH is presented and discussed, offering everyone a chance to learn from and teach each other.

Students in the nursing simulation lab at UNH. Courtesy photo.
For this first project, the team is focused on medications for addiction treatment. Doyle says this will help nurse practitioner students receive the hours and training needed to qualify for the federal waiver allowing them to prescribe such medications to those who need it. Additionally, it will offer training, support and guidance to those in practice who have their waiver, but may be hesitant taking on substance abuse patients for fear they lack the training.
Currier says she’s hopeful that as time goes on, there will be even more talk about ways people across disciplines and sectors can come together to find solutions. “I would love to see us get to the next page, and get some solutions in place.”
