
Federal officials are raising concerns about New Hampshire and eight other states they say are leading the country in terminating Medicaid coverage for children now that pandemic protections have ended.
According to the Centers for Medicare and Medicaid Services, New Hampshire ended coverage for 19,810 children between March and September, an 18 percent drop. Only South Dakota and Idaho had bigger decreases, each with a 27 percent drop, according to CMS.
State officials are pushing back, saying the number of children who lost Medicaid and could still be eligible is lower – 9,229 as of Tuesday – and the state is still trying to reach them. Until it does, they won’t know if they still qualify for the program.
The children fall into two groups: Nearly 6,530 were disenrolled because their parent or guardian did not respond to the Department of Health and Human Services’ multiple requests to have their child’s eligibility reviewed. For the rest, a parent or guardian began the review but didn’t complete it.
“They are the two groups (where) our efforts have not yet succeeded, and they could still succeed because Medicaid is an open program,” said state Medicaid Director Henry Lipman. The department has extended its “reopen” deadline to allow children who lost coverage in the last 120 days to get a review without having to complete a lengthy Medicaid application.

State and federal Medicaid officials are urging people to renew their Medicaid eligibility now that federal pandemic protections have ended. Failing to do so could end coverage even for those who qualify. (Screenshot)
Lipman said the count CMS released Monday is inflated because the agency is counting children differently than New Hampshire does, going to age 23 versus 18. People over 18 are eligible for adult Medicaid instead.
They are also misleading, Lipman said, because the federal data did not indicate why the state disenrolled children, including whether they no longer qualified because they were too old or lived in families whose incomes had increased beyond the limit, or because they moved to other insurance.
Lipman and Gov. Chris Sununu said CMS is also overlooking steps the state has taken to keep children covered.
Those include setting higher income-eligibility levels than most states; extending the amount of time families can challenge a denial and retain coverage; and making extensive efforts to reach families that have lost coverage because they failed to complete an eligibility review. It launched a pilot project that expands efforts to reach those who haven’t responded, potentially leaving them with no assistance even if they would qualify.
“I always felt that among my most important things I would do in my career would be how we manage this whole process,” Lipman said. “We don’t want to lose people who should be covered from coverage. That’s how I approached it and others in the department did as well.”
Sununu, who was one of nine governors to get a letter Monday from Xavier Becerra, secretary of the U.S. Department of Health and Human Services, warning that his agency would not hesitate to act if New Hampshire did not address its concerns, had a more pointed response.
“Yet another example of the federal government being completely out of touch with what’s happening on the ground,” Sununu said in a statement to the Bulletin. “New Hampshire is doing everything they asked for and more.”
State says it has prioritized children
Federal authorities have been watching states closely since March, when the end of the federal public health emergency allowed them to redetermine the eligibility of child and adult Medicaid beneficiaries since the pandemic’s start.
During the pandemic, states received extra money to keep people enrolled regardless of whether their income or other qualifying circumstances had changed. That is no longer an option.
New Hampshire was among a handful of states to begin redetermining eligibility in April, the first month possible. Lipman said the state’s early start on redeterminations makes a comparison to other states challenging. “I think it’s comparing apples and oranges and apricots and watermelons,” he said.
The state launched a massive public awareness campaign well before it reinitiated eligibility reviews, alerting people that they would lose coverage if they did not have their eligibility redetermined at the end of the federal public health emergency. His team continues that outreach, he said.
The department also prioritized children by doing their redeterminations later than adults, to give their families more time to complete the process.
Lipman said that as of Tuesday, nearly 75 percent, or nearly 81,330 children, who had Medicaid as of March 1 continue to be covered. The 25 percent, or 27,114, who lost coverage did so for one of several reasons.
Nearly 40 percent, or 10,798, were beyond the income limit because their family’s earnings had increased. About 7,090 no longer met Medicaid guidelines, such as reaching the age limit, or because their family told the department they no longer need the insurance.
The nearly 9,229 who lost coverage because their family has not completed an eligibility review may or may not still qualify for Medicaid. The department can’t know until it hears from them.
Lipman’s office has focused most heavily on that last group in hopes of continuing coverage for those who qualify and helping those who don’t find other affordable coverage, such as a subsidized plan on the Affordable Care Act Marketplace.
Lipman and Sununu pointed to the state’s strong economic rebound and low unemployment rate as another driver of lower Medicaid enrollments. They called them indicators that many families’ incomes have improved enough that they are no longer eligible for Medicaid.
State has followed federal guidance
On Monday, CMS suggested states take a number of steps to avoid ending Medicaid coverage for those who still qualify. New Hampshire has been doing many of them for months, a few for years.
- States, it said, should ensure a child’s eligibility be determined separate from their parents, because income limits are higher for children. The state Department of Health and Human Services began doing that in September, based on new guidance from CMS. As of late September, it had restored coverage for 1,351 and provided retroactive coverage for bills incurred during their pause in benefits.
- CMS urged states to use existing information to determine whether a child remains eligible for Medicaid, allowing them to keep coverage without having to do the redetermination process. Lipman said the state has long used data from the Supplemental Nutrition Assistance Program to identify children who qualify for automatic renewal.
- States with expanded Medicaid tended to see fewer disenrollments, CMS said. New Hampshire has had expanded Medicaid since 2014.
- CMS urged states to expand outreach by partnering with schools, health care providers, community-based organizations, and other groups that work with families. Lipman said his department has also given health care providers and insurance navigators information about who has not completed redeterminations as another way to reach them.
- States were encouraged to expand their call center to minimize the wait time for people trying to have their eligibility redetermined. Lipman said the department did so, adding 34 people.
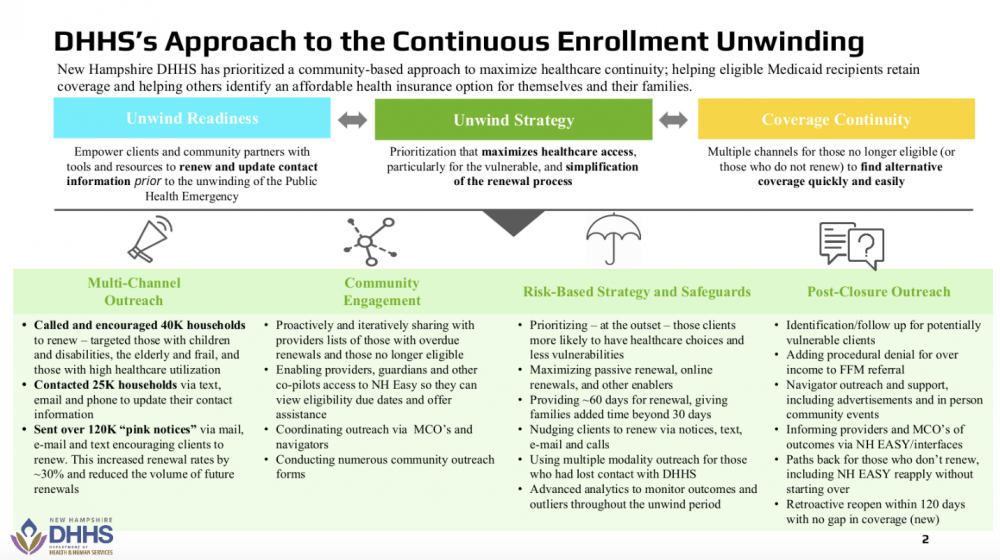
The Department of Health and Human Services’s effort to help qualified Granite Staters keep their Medicaid included contacting 25,000 households via text, email, and phone, targeting households with children and people who are older or have disabilities. (Screenshot)
MEDICAID RESOURCES
There are several resources for people with questions about maintaining their Medicaid.
Individuals can visit nheasy.nh.gov, the state’s online portal to government benefits and local services. The department can also be reached by phone at 1-844-ASK-DHHS (1-844-275-3447), or in person at one of the department’s local offices.
The state’s two federally funded health care “navigator” programs can also assist people with eligibility questions and insurance options, and help them buy a plan through the Affordable Care Act Marketplace. First Choice Services (firstchoiceservices.org) and Health Market Connect (hmcnh.com) both provide free assistance in multiple languages. The New Hampshire Insurance Department is another option.
