
Alfred Montoya working in his office at the Manchester VA Medical Center. Courtesy photo.
Alfred Montoya was at his son’s baseball game on a Saturday afternoon in Connecticut when he learned that in less than two days, he’d be starting a new job. “I received a phone call from our [Veterans Affairs] network office down in Bedford, Mass.,” he says, recalling that day in summer 2017 when he assumed the helm of the Manchester VA Medical Center as interim director. “They said, essentially, you need to go to Manchester on Monday.”
He got the call because that day, July 15, 2017, The Boston Globe published an article by journalists Jonathan Saltzman and Andrea Estes outlining a litany of problems at the Manchester VA Medical Center. The article, based on accounts from 11 Manchester VA doctors, staffers and administrators turned whistleblowers, depicted NH’s only veteran’s hospital as a place where:
• An operating room had to be shut down because of a recurring fly infestation.
• Surgeries were canceled because a substance (either rust or blood) was found on supposedly sterile operating instruments.
• Thousands of veterans—some with life-threatening illnesses—were waiting months to be seen by a doctor.
• Concerns from doctors about care, cleanliness and safety were ignored.
• Spinal patients did not get proper care to debilitating results.
The whistleblowers’ concerns prompted a January 2017 investigation by the U.S. Office of the Special Counsel, which concluded, according to the Globe, that there was a “substantial likelihood” the VA was guilty of legal violations, gross mismanagement, abuse of authority, and being a danger to public health. But only after the Globe article was published did federal officials from VA order a review of the hospital and remove Manchester’s director Danielle Ocker and her chief of staff James Schlosser.
“So my journey started here on the 17th of July,” Montoya says, “when I came to a medical center that really was in crisis.”
Setting a New Course for the VA
In the 15 months since, Montoya has worked to get the VA Medical Center back on track. He’s asked for and received federal funds to fix infrastructure, increase staff pay and make new hires. He’s streamlined cumbersome processes, created partnerships with community hospitals, established an academic relationship with Dartmouth’s Geisel School of Medicine and added new programs.
Montoya has also overseen the implementation of some of the 29 recommendations made by a task force composed of local and regional veterans’ advocates, two of the whistleblowers, and VA officials, among others, that assembled last year to assess changes needed at the Manchester VA to improve care and ensure such dereliction does not recur. “We’re not where we want to be yet,” Montoya says. “But we’re sure as heck a lot further than we were, and we’re continuing to make those leaps and bounds.”
When It Rains, It Floods
Montoya is a veteran of the U.S. Air Force, which included working as a Russian cryptologic linguist. He began his career with VA in 2009, serving over the years as an education coordinator, an executive assistant to the director, an assistant director and VA Medical Center director in White River Junction in Vermont. He had been on that job for two years when he was named interim director in Manchester.
Two days into his new job, he awoke at 4 a.m. to a call telling him there was a “leak” at the Medical Center on Smyth Road and he needed to come in right away. “A leak? It can’t be that bad,” Montoya says he thought at the time. “I’ve seen bad leaks before.”
But this wasn’t just a leak. This was a geyser of thousands of gallons of water from a broken pipe on the seventh floor of the Manchester facility. The water spread through administrative offices, operating rooms, the third floor, and the second floor destroying 61,000 square feet of the building, Montoya says.

The flood at the Manchester VA. Courtesy photo.
“You couple that with the Boston Globe article, with the chaos the organization was already facing, and it really sent the organization into a tailspin,” he says. “But looking back on it, I think the flood was maybe the best thing that could have happened to this campus because it brought all of us together as a team. And it also brought a lot of attention.”
Montoya says in the hours and days after the flood and closure of the affected areas, he began receiving calls from local health care providers asking how they could help provide care to the roughly 26,000 veterans who use the Medical Center.
They started redirecting veterans to those new local partners, he says, many of whom, such as Catholic Medical Center and the Elliot Hospital, have remained partners in the care of veterans even after the flood and reconstruction.

From left: Alex Walker, executive VP and COO of Catholic Medical Center (CMC); Joseph Pepe, president and CEO of CMC; Carolyn Clancy, Veterans Health Administration deputy undersecretary; and Alfred Montoya of the Manchester VA Medical Center. Local hospitals, such as CMC, have remained partners with the VA. Courtesy photo.
The flood caused $8.5 million in damage. The bulk of the repairs, as well as some upgrades—including installing energy-efficient lighting and improving the appearance of lobbies and welcome areas—was completed within 11 months, Montoya says. “This building was built in the 1950s, so there were some infrastructure changes that needed to happen; this [flood] helped with that process,” he says. There are still some ongoing projects, he says, including the replacement of the original chilled water pipe that broke.
What Went Wrong?
While dealing with the aftermath of the flood, Montoya also probed what went wrong at the Medical Center that caused the systemic failures reported by The Boston Globe. Among the causes, he says, was a lack of stable leadership for more than 10 years at the Manchester VA. A director would come in for a couple years, only to be replaced by another for a year, followed by an interim director, and so forth. “That doesn’t allow staff to grab onto certain priorities at the Medical Center,” he says. “The revolving leadership took its toll.”
The budget was a factor, Montoya says. He explains that the way the VA budgeting process works is budget decisions are handed down from D.C. to the networking office in Massachusetts and then to the eight medical centers in New England.
Those budgets are based on workload, which was dwindling at the VA in Manchester, so that led to smaller budgets over the years.
Despite being the only VA Medical Center in the state, it is not a full-service hospital. Patients requiring surgery or hospitalization go to other hospitals. Furthermore, during the past several years, some services the Manchester VA provided, such as cataract surgeries and nuclear cardiac stress tests, had ceased due to lack of staffing, tools or resources, the whistleblowers told the Globe.
Also at issue was the Veterans Choice Program—which had its own set of problems. It allowed VA patients to receive care almost anywhere they liked outside the VA system as long as they didn’t live within 20 miles of White River Junction or Dartmouth-Hitchcock Medical Center in Lebanon. “And so that essentially is everyone in New Hampshire,” Montoya says.
According to the Globe, the Manchester VA began to rely heavily on this program since it came with its own bucket of money, which allowed the Manchester VA to connect a veteran with a service without dipping into its own coffers.
Another problem was low morale among staff due in large part to employees feeling as though their concerns about quality of care and other issues were not being taken seriously. Ranking member of the House Veterans’ Affairs Subcommittee on Oversight and Investigations Rep. Annie Kuster, D-NH, and Sen. Jeanne Shaheen, D-NH, who sits on the U.S. Senate Committee on Armed Services, began looking into the troubles at the VA in 2016.
So with all this as backdrop and thousands of gallons of standing water at his feet, Montoya says on the third or fourth day on the job, he called his bosses in D.C.
“I was saying, ‘Look, I can fix this, but I need you guys to let me do it my way. I need you guys to give me the resources I need, and I need you to let me try creative things,” he says. “And the answer back was, ‘Al, we don’t care what you do, just get this under control.”
Listening to Stakeholders
Montoya says one of his first orders of business was to meet with stakeholders to find out what was going on. Montoya held monthly town meetings for veterans in different locations across the state, as well as twice-monthly, hour-long meet-and-greet sessions at the facility. He also engages employees by walking around the facility with a coffee cart twice a month to chat with them and holds formal town hall meetings for staff. He also attended meetings coordinated by the whistleblowers.
He started giving out his cellphone number at town hall meetings and to employees. He later held a veterans open house to celebrate the expansion of services at the VA, started a regular column in The Union Leader and made frequent appearances on a local veteran-focused radio show.

The VA open house featured demonstrations by Ron Currier, veteran bilateral LUKE Arm recipient, surrounded by his
Manchester VA support team and Matt Albuquerque of Next Step Bionics & Prosthetics, third from left. Courtesy photo.
Montoya says this was critical to clarify the problems and to start rebuilding trust among the organization and its staff, the veterans and the community.
It seems to be working. “I’ve been able to witness and certainly have heard in my conversations with staff and veterans that there has been a pretty dramatic cultural shift,” says U.S. Rep. Annie Kuster. “The relationship with the congressional delegation has greatly improved. We were always in constant contact with previous leadership, but I think you have to give him credit for being more responsive.” Shaheen says of Montoya’s efforts to reflect a new philosophy of transparency at the agency.
New Leadership Team
Another priority for Montoya was amassing a new leadership team since the top two administrators were relieved of their duties after the Globe article came out and the head nurse was retiring.
“I was able to recruit a nurse executive from a higher-complexity facility because she believes in what we’re doing and the direction we’re headed,” he says, speaking of Bernadette Jao, associate director of Patient and Nursing Services at the Manchester VA. “I was also able to recruit Paul Zimmerman to come aboard as the chief of staff.” Zimmerman has a long career with the VA, most recently serving as acting chief of quality management and deputy associate chief of staff for medical and dental education.
“Seventy-five percent of my senior leadership team are veterans,” he says. “And 32 or 33 percent of our entire workforce of 850 employees are also veterans. And that makes a huge difference,” he says. Montoya notes that as a veteran, he receives all of his medical care at the VA.
Next Steps
With the first two prongs—rebuilding the leadership team and restoring trust—of a five-pronged strategy under way, Montoya says his team has started implementing the rest of the plan: improving care, fixing the Choice Program and designing the future.
To improve care, Montoya says they evaluated all current programs to see where they could add more services and providers. “We wanted to help veterans choose the Manchester VA,” he says. “So, if you’re in a state where essentially every veteran can pick up a phone and go out in the community [for care], you have to make it a point to say how do I make the services that we provide here even better than they are in the community.”
Also, if the Manchester VA can show it is providing more services to more veterans in-house, it will mean budget dollars coming into its coffers rather than to outside providers.
The Manchester VA hired an ophthalmologist, so it can once again do cataract surgeries on-site. “It’s been, some say, two to three years since we’ve done cataract surgeries here. In fact, we still have the equipment,” Montoya says. The Manchester VA has also added a new allergy clinic.
Manchester VA officials examined wait times that veterans were experiencing just to see a primary care doctor. Montoya says veterans who were new patients were waiting an average of 77 days largely because the VA was understaffed. “Of the 36 primary care teams that we had, roughly 90 percent of them were overpaneled,” he says, explaining that a primary care provider would have roughly 1,200 veterans assigned to them. “They were all over by about 110, 120, 130 percent,” he says.
To alleviate this, Montoya hired more primary care doctors and gave raises to the ones he had. He says wait times for new patients for primary care are now 19.7 days.
“That’s a reduction of 50-some days, by investing in your staff, by paying them appropriately. In some cases, I had primary care providers that for the life of me, I couldn’t figure out why they stayed,” Montoya says. “The turnover rate in primary care providers was one of the biggest complaints I got from veterans at that first town hall.”
Kristin Pressly, a spokesperson for the Manchester VA Medical Center, says since July 2017, staff has increased by 66 full-time-equivalent employees, but she adds, “the number of staff is a moving target, as we are constantly adding and repurposing staff to best meet the needs of veterans as well as staff up emerging programs.”
The Manchester VA also hired two respiratory therapists, four physical therapists, an occupational therapist, 18 registered nurses, seven physicians, two pharmacists, a physician assistant, an optometrist, and the equivalent of 2.7 social workers, 1.5 audiologists, and 4.2 nurse practitioners. It also hired a full-time suicide prevention coordinator as suicide rates among veterans is high. The VA has committed to a zero suicide initiative. Plus, it is adding administrative staff to support the additional clinical staff.
The Manchester VA team also had to ensure that staff was following required administrative procedures. For veterans who are seen at the VA for a non-service-related injury, by law the VA is required to collect that patient’s third-party insurance information to bill for that service.
“Out of a budget of about $200 million, that makes up about $12 million of my budget,” Montoya says. “System-wide, we were collecting that [insurance information] only about 40 percent of the time. That started a whole process,” he says, and resulted in insurance cards being collected in 92 percent of cases in July. The Manchester VA also trains staff to code visits correctly, which can affect the budget down the line.
Next, Montoya says, his staff is attempting to address problems with the Veterans Choice Program. According to the Globe article, the program, which enjoys a less-than-stellar record across the country, was especially bad in NH, mainly because the hospital had cut so many services and referred so many patients.

Herman “Herk” Streitburger, a WWII veteran and former prisoner of war, celebrates his 99th birthday with, from left, Sarah Craig, POW program coordinator, and VA volunteers Sheila Peters and Madeline Dreusicke. Courtesy photo.
The Globe article also stated, “Choice, which is administered by Health Net Federal Services, failed to make some 3,100 appointments requested by Manchester veterans in the first five months of [2017], according to a VA document obtained by the Globe. That was easily the worst record of the eight VA Medical Centers in New England and included hundreds of patients who have been waiting more than six months, some with life-threatening conditions.”
Montoya explains that at the time, the Manchester office had 10 people to handle all of the consults and referrals from every veteran in the state who was eligible to use Choice. Within a few weeks, Montoya says, he recognized that there were at least 300 consults or referrals that required action.
To address this, the VA engaged outside consultants from systems that were actually working and created a case management system. Now, he says, there are 27 employees on six teams that handle those consults and referrals, with each team responsible for a specific type of care, such as physical therapy. Manchester VA also hired a primary care-trained physician to oversee those teams. Montoya says the VA also stopped using Health Net about six months ago, although it still has a contract with that company through the end of September.
The VA hired a provider relations specialist to sort out what the VA owes, pay those bills in a timely manner, and determine what, if anything, the VA might be owed. The specialist also meets with providers to address any problems they may have, he says.
Task Force Recommendations
On Aug. 4, 2017, then-U.S. VA Secretary David Shulkin created the VA NH Vision 2025 Task Force, a group of veterans’ advocates, VA whistleblowers, VA officials and executives from private healthcare organizations in NH. The job of the task force was to develop “a vision for VA care delivery in the state that would best meet the needs of veterans now and in the future,” and could be implemented by 2025. Its work resulted in 29 recommendations for improving the Manchester VA, despite several changes in VA representation on the task force and changes in leadership at the national level.
The task force’s recommendations addressed everything from organizational issues to improving and growing specialty care such as mental health and addiction treatment, pain management and radiology services. There were also recommendations to create a regional center of excellence for amputation care; merge outpatient clinics on the Seacoast; create a whole-health community center in Manchester; provide telehealth services; and establish an ambulatory care center in Manchester.
The Manchester VA’s approach to improvement has caught the attention of other VA officials. “The model is already becoming a model for the rest of the country,” says task force co-chair Jennifer MacDonald. “I will say that they are far ahead of the [2025] time frame,” she says. “And by the time we presented the recommendations, they had started or achieved many of [them].”
For example, the task force wanted the Manchester VA to invest in the organization’s culture. Montoya says this year the Manchester VA is focused on communication, growth, workload and “psychological safety” for employees—the ability to raise concerns without fear of retribution. A member of the executive leadership team has been assigned to head up efforts in each of those categories, working with frontline employees and emerging leaders to take ideas generated by employees and put them into action, Montoya says.
When it comes to improving the veteran experience, Montoya says they have expanded hours and added a second employee each to the patient advocate team and the suicide prevention program.
Montoya says they’ve also obtained a $400,000 grant and started a whole-health initiative that includes programs and services such as yoga, acupuncture, tai chi and meditation. The Medical Center has partnered with community YMCAs, which will offer space for the yoga classes and allow veterans to use the rest of the facilities for free that day. More than 750 veterans have already taken yoga classes. The Center also established an outpatient recreational therapy program for vets that will include snowboarding, skiing, surfing and kayaking.
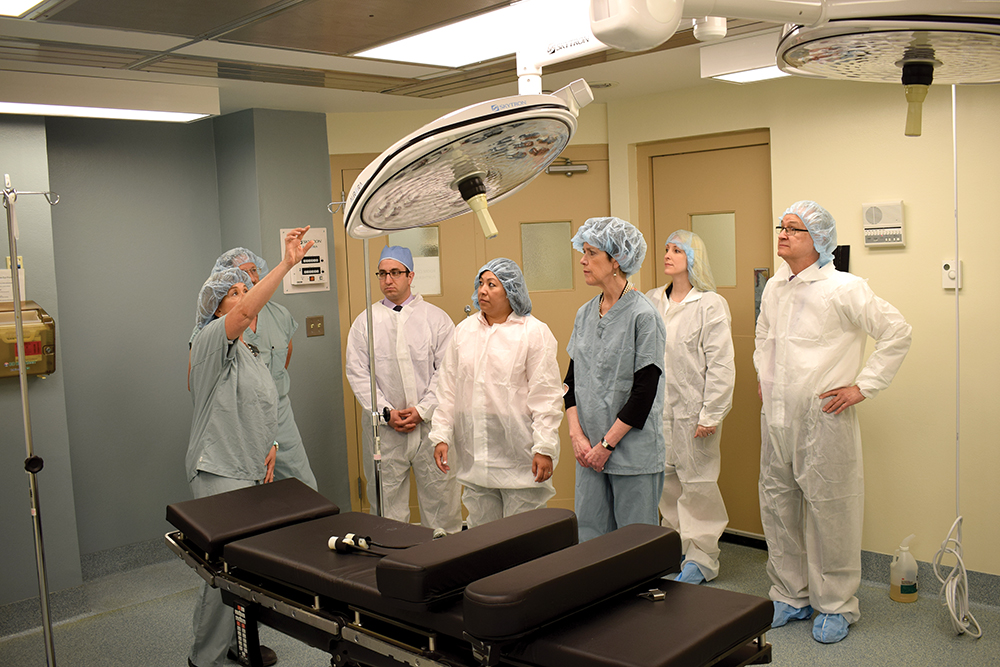
Dr. Bernadette Jao, fourth from right, and colleagues in the newly reopened operating room. Courtesy photo.
Also in the works is a whole-health center, which will house mental health services, including support staff and resources to help address issues of homelessness, substance abuse and legal problems. Montoya says they are in talks with community partners about securing space.
Before the end of the year, he anticipates the Manchester VA will sign an academic affiliation agreement with Dartmouth, which will allow residents and students to work and train at the VA.
Some of the whistleblowers have mixed feelings about the progress of the VA. Stewart Levenson, MD, a whistleblower who is running for U.S. Congress says while some progress has been made, there is more to accomplish. “It has always been my belief that the VA provides excellent care to the majority of its patients but that is poor conciliation to those who fall through the cracks. Much more needs to be accomplished before we as Americans can say we are keeping our promise to our veterans,” he says.
William “Ed” Kois, head of Manchester VA’s spinal cord clinic, is another whistleblower. He says new leadership has greatly improved communication within the center.
“There had been a total shutdown of communications between the staff and the powers that be. We had a number of physicians, who had significantly important positions, leave because they didn’t feel they were being heard,” Kois says. That has changed, he adds.
Kois agrees there is still work to be done, but says progress is being made and staff and management are working together rather than against each other.
Kois says the problems are far from limited to the Manchester VA. “I think we’ve got to change the whole culture of the VA.
And one of the things I testified to before Congress was that we should be using the Manchester VA as a beta site for the way that the VA changes,” he says. Kois credits leadership with making the Manchester VA less isolated and creating partnerships in the community, which make it more accountable.
Could This Happen Again?
Kuster, Shaheen and U.S. Sen. Maggie Hassan all say there will be continued legislative oversight of the VA. But the legislature has always had that capability and responsibility, and while several lawmakers began looking into issues at the VA in late 2016, changes didn’t come about until the problems were made public in the press through whistleblowers.
Hassan says she’s hoping the Mission Act will lead to further oversight of VA facilities. The bipartisan legislation was signed into law earlier this year and lays out a mandate for, among other things, allowing veterans to receive care outside the VA and is supposed to fund that care.
Montoya says that the Manchester VA has submitted to roughly 65 visits from independent agencies conducting surveys over the course of the year. Montoya also points to the tri-annual accreditation process by The Joint Commission, which analyzes VA facilities, as another layer of external oversight. But the problems brought to light last summer had been around for years and didn’t affect the accreditation of the facility. In 2016 the Veterans Affairs Department raised Manchester’s quality rating—a place with a fly infestation in the OR—from three stars to four, according to the Globe report.
In the end, Montoya says, the VA is responsible for making sure veterans are receiving the care they should. “I think we take that ownership for that on ourselves. It’s about getting out there and being transparent. We’re in a lot better place than where we were,” he says.
Ultimately, he hopes the systems and processes he’s helped establish will remain long after he’s gone. “Now are we going to get it right every time? No. But that’s when we go back and look at the process,” he says. “What step did we miss in the process, so we can readjust and do it better? How you keep this from happening in the future is you put the processes in place that make it replicable every single time.”

 Current Issue - April 2024
Current Issue - April 2024